Impacted Teeth
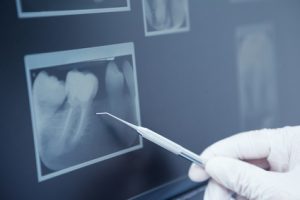 An impacted tooth simply means that it is “stuck” and cannot erupt into function. Patients frequently develop problems with impacted third molar (wisdom) teeth. These teeth get “stuck” in the back of the jaw and can develop painful infections among a host of other problems. Since there is rarely a functional need for wisdom teeth, they are usually extracted. Frequently, there are teeth other than wisdom teeth become impacted. These teeth generally cannot be extracted, since they are potentially functional and many times vital to overall long term oral health.
An impacted tooth simply means that it is “stuck” and cannot erupt into function. Patients frequently develop problems with impacted third molar (wisdom) teeth. These teeth get “stuck” in the back of the jaw and can develop painful infections among a host of other problems. Since there is rarely a functional need for wisdom teeth, they are usually extracted. Frequently, there are teeth other than wisdom teeth become impacted. These teeth generally cannot be extracted, since they are potentially functional and many times vital to overall long term oral health.
The maxillary cuspid (upper eyetooth)
Next to wisdom teeth, upper cuspids are the second most common teeth to become impacted, since they are the last functional teeth to erupt in the upper arch. The cuspid tooth is critical in the dental arch and plays an important role in your “bite”. They are very strong and have the longest roots of any human teeth. They are designed to be the first teeth that touch when your jaws close together so they guide the rest of the teeth into the proper bite. Therefore, it is always advantageous to retain these teeth rather than extract them.
Normally, the maxillary cuspid teeth are the last of the “front” teeth to erupt into place. They usually come into place around age 13 and cause any space left between the upper front teeth to close together. If a cuspid tooth gets impacted, every effort must be made to get it to erupt into its proper position in the dental arch. The techniques involved to aid eruption can be applied to any impacted tooth in the upper or lower jaw, but most commonly they are applied to the upper cuspid teeth. Sixty percent of these impacted eyeteeth are located on the palatal (roof of the mouth) side of the dental arch. The remaining impacted cuspids are found in the middle of the supporting bone but stuck in an elevated position above the roots of the adjacent teeth or out to the facial side of the dental arch.
The second molars
The second molars are the teeth directly in front of the wisdom teeth. In some patients with small jaws and large teeth (or a combination of both), the second molars as well as the wisdom teeth might become impacted due to a lack of space. These are difficult clinical scenarios, since the only solution is to wait for the patient to continue growing to allow the space for the second molars to erupt. During this time, the partially submerged second molar will be difficult to maintain and clean, resulting a high risk of infection. A possible treatment would be to expose the second molars while removing the wisdom teeth.
Timing
The older the patient, the more likely an impacted teeth will not erupt by nature’s forces alone even if the space is available for the tooth to fit in the dental arch. The American Association of Orthodontists recommends that a panoramic screening x-ray, along with a dental examination, be performed on all dental patients at around the age of seven years to count the teeth and determine if there are problems with eruption of the adult teeth. It is important to determine whether all the adult teeth are present or are some adult teeth missing.
This exam is usually performed by your dentist or hygienist who will refer you to an orthodontist if a problem is identified. Treating such a problem may involve an orthodontist placing braces to open spaces to allow for proper eruption of the adult teeth. Treatment may also require referral to an oral surgeon for extraction of over-retained baby teeth and/or selected adult teeth that are blocking the eruption of the impacted tooth. The oral surgeon will also need to remove any extra teeth (supernumerary teeth) or growths that are blocking eruption of any of the adult teeth. If the eruption path is cleared and the space is opened up by an early age, there is a good chance the impacted tooth will erupt spontaneously. If the impacted tooth is allowed to develop too much, it will not erupt by itself even with the space cleared for its eruption. Therefore, the key is early intervention and treatment before the roots have fully formed.
Treatment
In cases where the impacted tooth will not erupt spontaneously, the orthodontist and oral surgeon work together to help these unerupted teeth to erupt. Each case must be evaluated on an individual basis but treatment will usually involve a combined effort between the orthodontist and the oral surgeon. The most common scenario will call for the orthodontist to place braces on the teeth. Next, a space will be opened to provide room for the impacted tooth to be moved into its proper position in the dental arch..
The gums on top of the impacted tooth will be lifted up to expose the hidden tooth underneath. If there is a baby tooth present, it will be removed at the same time. Once the tooth is exposed, the oral surgeon will bond an orthodontic bracket to the exposed tooth. The bracket will sometimes have a miniature gold chain attached to it. Once the tooth exposed and brackets are placed, the surgeon will leave the exposed impacted tooth completely uncovered by suturing the gum up high above the tooth or making a window in the gum covering the tooth. Other times, the gum will be returned to its original location and sutured back with only the chain remaining visible as it exits a small hole in the gum.
Shortly after surgery (1-14 days) the patient will return to the orthodontist. A rubber band will be attached to the chain to put a light eruptive pulling force on the impacted tooth. This will begin the process of moving the tooth into its proper place in the dental arch. This is a carefully controlled, slow process that may take up to a full year to complete. Remember, the goal is to erupt the impacted tooth and not to extract it. Once the tooth is moved into the arch in its final position, the gum around it will be evaluated to make sure it is sufficiently strong and healthy to last for a lifetime of chewing and tooth brushing. In some circumstances, especially those where the tooth had to be moved a long distance, there may be some minor “gum surgery” required to add bulk to the gum tissue over the relocated tooth so it remains healthy during normal function. Your dentist or orthodontist will make this recommendation to you if it applies to your specific situation.
Anesthesia and Recovery
The surgery to expose and bracket an impacted tooth is a surgical procedure that is performed in the oral surgeon’s office. For most patients, it is performed under IV sedation if the patient wishes to be asleep. For patients with mild to moderate anxiety, this route is recommended.
You can expect a limited amount of bleeding from the surgical sites after surgery. Although there will be some discomfort after surgery at the surgical sites, most patients find Ibuprofen or Advil to be more than adequate to manage any pain they may have. Within two to three days after surgery there is usually little need for any medication at all.
Your doctor will see you seven to ten days after surgery to evaluate the healing process and make sure you are maintaining good oral hygiene. You should plan to see your orthodontist within 1-14 days to activate the eruption process by applying the proper elastic traction to the chain on your tooth.
